Chronic Lower Back Pain: The Biopsychosocial Approach
Index
Spine structure includes vertebrae, disks, and nerves; injuries cause chronic pain.
Neurological processes significantly influence the perception of chronic pain.
Muscle strength and flexibility are vital for preventing chronic back pain.
Chronic inflammation contributes to ongoing low back pain and affects quality of life.
Psychological factors like stress can worsen chronic pain experiences.
Social support networks are essential for managing chronic pain effectively.
Socioeconomic status affects access to treatment for chronic pain sufferers.
Cultural beliefs influence pain perception and treatment-seeking behavior.
Social media can provide support but also spread misinformation about pain management.
Family dynamics impact how individuals express and cope with chronic pain.
The biopsychosocial model facilitates comprehensive understanding and treatment of chronic pain.
Psychological influences significantly affect pain perception and treatment effectiveness.
Social context plays a crucial role in managing chronic lower back pain.
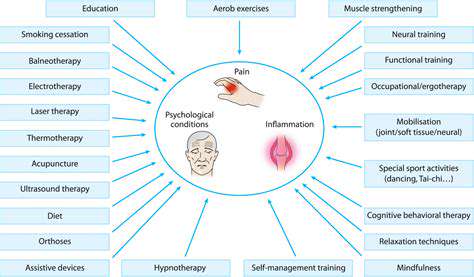
Integrated treatment approaches combine physical, psychological, and social strategies for better outcomes.
Patient education enhances self-management and treatment adherence for chronic pain.
Future research in biopsychosocial factors aims to improve chronic pain treatments.
The Biological Aspects of Chronic Lower Back Pain

Understanding the Anatomy of the Spine
- The spine is composed of vertebrae, disks, and nerves that work together.
- Disruptions in this structure can lead to chronic pain conditions.
- Components such as muscles and ligaments play a critical role in spinal health.
The human spine is a complex structure made up of 33 vertebrae, intervertebral discs, ligaments, and numerous muscles that support its function. Each vertebra is stacked upon another, creating a durable yet flexible column that enables various movements. When this intricate system faces injury or degeneration, such as herniated discs or osteoarthritis, it can lead to Chronic lower back pain, persisting for weeks or even years.
Additionally, the intervertebral discs act as shock absorbers, allowing for movement and flexibility while preventing vertebrae from grinding against each other. Should these discs degenerate, they can lose height, causing misalignment and pressure on spinal nerves, leading to discomfort and pain.
Neurological Contributions to Pain Perception
The perception of pain is not solely about physical injury; it’s heavily influenced by neurological processes. The spinal cord and brain work together to interpret signals from injured tissues, and this interaction can exacerbate or diminish the experience of pain. Certain neurotransmitters, like substance P and glutamate, play significant roles in escalating pain sensations, indicating why the same injury may result in different pain experiences among individuals.
Moreover, studies show that chronic pain can lead to changes in brain structure itself, notably in areas involved in emotional regulation and pain processing. This neuroplasticity means that Chronic Lower Back Pain is not just a physical ailment, but rather a condition that often involves both physiological and psychological dimensions.
The Role of Musculoskeletal Health
- Muscle strength and flexibility directly influence back health.
- Adequate physical activity can mitigate the risks of chronic back pain.
- Muscle imbalances can contribute to pain conditions.
Strong, flexible muscles surrounding the spine are essential for maintaining good posture and supporting the body's movements. Weakness or stiffness in these muscles can increase the risk of injuries, leading to pain that persists over time. It’s essential for individuals, especially those with sedentary lifestyles, to engage in regular exercise aimed at strengthening the core and back muscles.
Moreover, research highlights that individuals with chronic lower back pain often exhibit muscular imbalances that can perpetuate their condition. Implementing a tailored program of strength training and stretching can be beneficial in restoring balance and reducing pain.
Inflammation and its Impact on Chronic Pain
Inflammation is one of the body’s natural responses to injury, but when it becomes chronic, it can contribute significantly to prolonged pain. In cases of chronic lower back pain, inflammation may stem from various conditions like disc disease, arthritis, or muscle strain. This persistent inflammation results in ongoing pain signals that can severely affect an individual’s quality of life.
Recent studies suggest that inflammatory markers, such as C-reactive protein (CRP), are often elevated in patients suffering from chronic pain conditions. Addressing inflammation through medical interventions, such as physical therapy or medication, can significantly alleviate symptoms and improve overall health.
Psychological Factors Influencing Pain Management
Chronic lower back pain is not only a physical problem but also heavily influenced by psychological factors like stress, anxiety, and depression. These mental health conditions can create a vicious cycle, where pain leads to increased anxiety and depression, which, in turn, can intensify the perception of pain. Understanding this Biopsychosocial Model is crucial for effective pain management.
Furthermore, cognitive behavioral therapy (CBT) has been shown to be effective in helping patients manage chronic pain by changing negative thought patterns associated with their condition. Therapists work with individuals to develop coping strategies and to emphasize psychological resilience, which may help reduce the intensity of their pain experience.
The Psychological Dimensions of Pain
The Neurobiological Impact of Chronic Pain
Chronic pain not only affects the body but also alters brain structure and function. Research indicates that persistent pain can lead to changes in the grey matter volume, especially in areas responsible for emotion regulation and pain perception. A study conducted by Apkarian et al. (2004) revealed that patients with chronic back pain show significant alterations in brain structure, suggesting that long-term pain might embed itself within the neurobiology of pain processing.
Moreover, neuroimaging studies demonstrate that chronic pain conditions are often associated with increased activity in brain regions such as the anterior cingulate cortex and insula. These areas are crucial for processing emotions and making cognitive assessments regarding pain. Clinicians must recognize that treating chronic lower back pain might go beyond physical interventions and involve addressing these neurobiological changes, potentially through cognitive-behavioral therapies or pharmacological approaches that modulate pain perception.
The Role of Psychological Factors in Pain Perception
Psychological factors significantly influence how individuals perceive and cope with pain. For instance, anxiety and depression can exacerbate the experience of pain, creating a cycle that is hard to break. Research has shown that patients with lower back pain who also exhibit high levels of anxiety report greater pain intensity and a lower quality of life. This highlights the need for a biopsychosocial approach that recognizes the interplay between mental health and pain management strategies.
Additionally, cognitive appraisal, or how one interprets pain stimuli, plays a critical role. For example, those who view pain as a threat may experience more significant distress and disability compared to individuals who perceive it as manageable. Incorporating psychological assessments into pain management programs can enhance treatment outcomes. Exploring techniques such as mindfulness and acceptance-based therapies can assist patients in developing healthier coping mechanisms, ultimately fostering resilience against chronic pain's psychological burden.
The Social Influences on Chronic Pain
Understanding Social Circles and Chronic Pain
Social Support plays a crucial role in managing chronic pain. Close connections with family and friends can significantly alleviate feelings of isolation. Individuals who perceive strong emotional backing typically report lower pain levels and improved coping strategies. Researchers discovered that social networks can either buffer the negative effects of chronic pain or exacerbate its impact, depending on the nature of these connections.
Social circulations can discourage maladaptive behaviors, such as avoiding physical activity due to pain. Encouragement from peers to engage in light exercise or attend social events often prompts individuals to push past their discomfort, which is vital for recovery. Furthermore, the joy derived from positive social interactions can bolster one’s mental health, often resulting in a decrease in perceived pain levels.
The Impact of Socioeconomic Status
Socioeconomic Status (SES) is a significant determinant of health outcomes, including chronic pain experiences. Individuals from lower SES backgrounds often face barriers in accessing healthcare services, leading to underdiagnosing and undertreatment of chronic conditions. A study published in the Journal of Pain found that lower SES correlates with heightened pain levels and diminished psychological well-being.
Moreover, financial strain can create a cycle where patients become increasingly frustrated and helpless about their condition. This sense of isolation can lead to a negative feedback loop, worsening their pain experience. It's crucial for health professionals to consider these socioeconomic factors when evaluating treatment plans to ensure comprehensive care.
Cultural Perspectives on Pain
Cultural beliefs shape how individuals perceive and respond to pain. In some cultures, expressing pain is viewed as a weakness, which may discourage individuals from seeking necessary medical help. This cultural stigma can complicate treatment and lead to the under-reporting of pain, thereby impacting effective management. Variations in pain perception and expression across cultures highlight the need for culturally sensitive approaches in pain management.
For instance, in collectivist societies, chronic pain experiences may be communicated more subtly within the group dynamics rather than overtly expressed. Understanding these cultural frameworks is essential for healthcare providers employing a biopsychosocial approach as they develop targeted treatment strategies that resonate with diverse patient backgrounds.
Additionally, educational interventions that educate communities about modern pain management approaches can help challenge and refine traditional beliefs, allowing patients to find a balanced view on how to handle chronic pain. This approach not only improves individual treatment outcomes but also promotes a healthier community dialogue surrounding chronic pain.
The Role of Social Media
Social media platforms can serve as double-edged swords for individuals living with chronic pain. On one hand, they provide a community space for individuals to share their experiences and gain support from others who understand their struggles. Support groups formed online often offer emotional relief and practical advice, making patients feel less isolated in their journeys.
However, social media can also amplify negativity and misinformation. Users may encounter harmful narratives regarding pain management, which can lead them to unsuitable treatments or reinforce hopelessness. As a professional, it’s advisable for individuals to rely on verified information and seek guidance from qualified healthcare providers rather than basing decisions on social media discussions alone.
Family Dynamics and Pain Perception
Family environments heavily influence how an individual experiences and expresses chronic pain. Supportive families that encourage open discussions about pain and its effects foster a healthy outlook on coping strategies. In contrast, families with negative dynamics may inadvertently increase their loved one's perception of pain through invalidation or overprotection. Understanding these dynamics is vital for providers to create effective treatment environments.
Engaging family members in the treatment process can enhance compliance with treatment regimens. Encouragement from family can aid in recovery methods, such as physical therapy or psychological counseling. It’s helpful for healthcare providers to guide families in understanding their roles while respecting the patient’s autonomy, enhancing the management of chronic lower back pain.
Integrating the Biopsychosocial Model in Treatment
Understanding the Biopsychosocial Model
The biopsychosocial model is a holistic approach that considers biological, psychological, and social factors in the assessment and treatment of chronic conditions, such as lower back pain. By integrating these diverse dimensions, healthcare professionals can formulate a more thorough understanding of a patient's experience and health. Each factor interacts and influences one another, which is critical in developing personalized treatment plans.
Recent studies, such as those published in the Journal of Pain Research, highlight that effective management of chronic pain calls for a multifaceted perspective rather than a purely biomedical approach. For example, recognizing the role of emotional factors in pain perception can lead to more effective interventions and improved patient outcomes.
Role of Biological Factors
Biological factors include the physiological aspects of lower back pain, such as anatomy, injuries, and underlying conditions like arthritis. Healthcare providers assess these factors by utilizing imaging techniques like MRI and X-rays to identify structural issues that may contribute to pain. However, it’s essential to remember that imaging results do not always correlate with pain severity.
Research has demonstrated that even in cases of significant radiological findings, patients may not experience corresponding pain. This phenomenon emphasizes the importance of understanding that chronic pain is not solely determined by physical conditions. Adopting a biopsychosocial lens allows us to prioritize individualized treatment plans that encompass more than just biological interventions.
Psychological Influences on Pain
Psychological elements are paramount in the biopsychosocial schema, influencing an individual's perception of pain and their response to treatment. Factors such as stress, anxiety, and depression can heighten pain levels or even contribute to chronic pain syndromes. Therapeutic modalities, including cognitive-behavioral therapy (CBT), have shown efficacy in managing these aspects.
Current evidence indicates that addressing psychological barriers can enhance a patient’s coping mechanisms and quality of life. Programs that incorporate mindfulness and relaxation techniques have been backed by studies published in the Pain Management journal, demonstrating their impact on reducing perceived pain intensity.
Potential barriers to effective treatment include a patient's mental state and their beliefs about pain, making psychological assessments a crucial step in the pain management process.
The Social Context of Chronic Pain
Social factors encompass the environmental and cultural contexts that affect a patient's health and well-being. Socioeconomic status, access to healthcare, and social support networks can significantly influence one's experience with chronic lower back pain. For instance, individuals with strong social support often report better pain management outcomes.
A 2016 study in the American Journal of Orthopedics found that community support systems and family dynamics play vital roles in recovery and coping. Professionals must engage with patients' social environments by incorporating family members into treatment discussions, which can facilitate better adherence to treatment plans.
Integrated Treatment Approaches
Integrating various treatment modalities is vital for effective management of chronic lower back pain. This may include pharmacological treatments for biological pain relief, psychological interventions appropriate for emotional support, and social strategies that augment recovery. A collaborative approach among healthcare providers is critical, allowing for comprehensive patient care.
Techniques such as interdisciplinary pain management programs combine physical therapy, psychological counseling, and nutritional guidance. According to findings from the Mayo Clinic, these integrated programs can lead to more successful outcomes, enhancing patients' overall quality of life.
Patient Education and Self-Management
Educating patients about the biopsychosocial model is essential for effective treatment. When patients understand the multifactorial nature of their pain, they may take a more active role in their treatment, which has been shown to improve adherence and outcomes. Self-management strategies, such as mindfulness and exercise, empower patients to handle their symptoms proactively.
Educational resources, like workshops and informational brochures, can be instrumental in providing patients with the knowledge they need. A study published in the Pain Research & Management journal emphasizes the importance of tailored educational interventions in enhancing patients' understanding of their conditions and improving self-efficacy in pain management.
Future Directions in Biopsychosocial Research
The future of treating chronic lower back pain lies in advancing biopsychosocial research. Understanding how these three domains interact provides a fertile ground for discovering new treatment pathways. Researchers are leveraging technology, such as telemedicine, to conduct studies on patient outcomes in various contexts and demographics.
Innovative approaches, such as virtual reality therapy for pain management, are emerging from ongoing research and show promise in altering pain perception. Continued exploration of the biopsychosocial model can lead to novel interventions, making it essential for healthcare providers to stay informed and adaptable to new findings.
Read more about Chronic Lower Back Pain: The Biopsychosocial Approach
Hot Recommendations
-
*Health Tips for Gamers (Ergonomics, Eye Strain Prevention)
-
*Best Tips for Incorporating More Sunlight Into Your Day
-
*Guide to Practicing Minimalism for Less Stress
-
*Best Exercises for People with Asthma
-
*Understanding ADHD in Adults
-
*Guide to Managing Irritable Bowel Syndrome (IBS) Through Diet
-
*Understanding Osteoarthritis vs Rheumatoid Arthritis
-
*Health Tips for Men's Prostate Health
-
*Best Nutrition for Building Muscle in Your 40s+
-
*Best Tips for Creating a Peaceful Bedroom Environment
![Guide to Training for a Triathlon [Beginner Plan]](/static/images/26/2025-05/Running3ALayingtheGroundwork.jpg)


![How to Recover Faster After Workouts [Tips & Techniques]](/static/images/26/2025-07/ListentoYourBody3ARecognizingandAddressingSignsofOvertraining.jpg)





